mitechnology
The Bigger Picture: Ultra-Widefield Imaging in Medical Retina Care
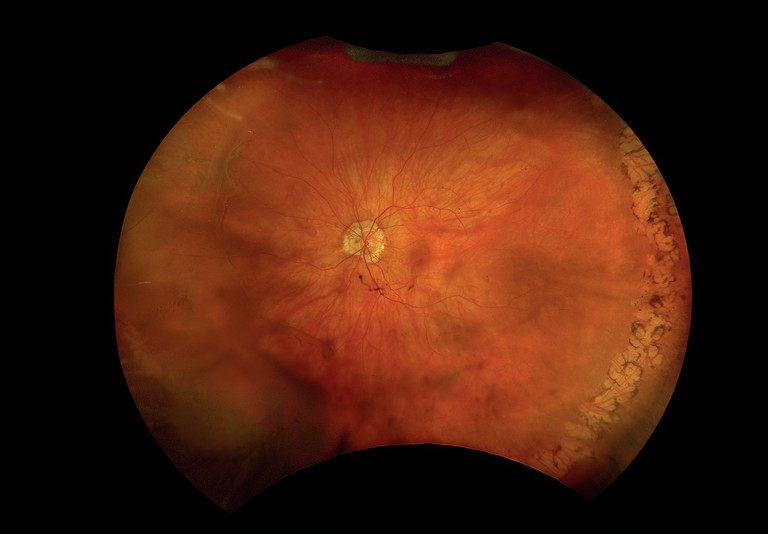
Above and right: Images captured using optomap ultra-widefield device.
For busy medical retina specialists, every minute in the consultation room counts. Sydney-based ophthalmologist Dr Peter Heydon explains how Optos optomap ultra-widefield imaging has become the cornerstone of his practice – accelerating diagnosis, strengthening the optometrist-ophthalmologist relationship, and involving patients in their own care.
WRITER Melanie Kell
Walk into a busy medical retina clinic and the pressure is immediately apparent. Patients present with acute symptoms, chronic disease requiring long-term monitoring, and everything in between. The challenge for any specialist is to be thorough, efficient, and communicative – often simultaneously. For Dr Heydon, a consultant ophthalmologist with subspecialty interests in medical retina and uveitis, optomap ultra-widefield (UWF) imaging has become integral to meeting that challenge.
“The major advantage is that you can identify pathology early on in the workup and consultation,” said Dr Heydon. “Before the patient has even entered the room, if they’ve presented with blurred vision, I’ll look at the optomap (taken by my orthoptist) and I might have already identified they’ve got a branch retinal vein occlusion – or they might present with floaters and I’ve seen the retinal tear. It just improves the efficiency of the consultation because I know immediately what treatment we’re going to offer, and we can spend more time talking about that.”
SEEING FURTHER, ACTING FASTER
The ability to image up to 200° of the retina in a single capture – compared with the 90° offered by older systems – has direct clinical consequences. In diabetic retinopathy, for example, neovascularisation can develop well outside the traditional field of view, meaning it has historically been missed until it reaches a more threatening stage.
“It’s often on ultra-imaging that we can detect areas of neovascularisation that we might not have seen previously. It can certainly help me get the correct grade of diabetic retinopathy and the level of severity, and that can be important in terms of the patient’s treatment and prognosis.”
For his uveitis patients, the wide field of view is equally valuable. Peripheral vascular leakage – a key indicator of intraocular inflammation – is now visible in a way that was previously difficult to visualise with clinical examination and older camera and angiography systems. “The ultra-widefield view allows me to see vascular leakage right out in the periphery, and that can be very important in gauging the level of inflammation and guiding treatment,” he said. In acute settings, he has used optomap to diagnose peripheral retinitis in acute retinal necrosis – one of the most time-critical ocular emergencies.
BRIDGING THE GAP BETWEEN OPTOMETRY AND OPHTHALMOLOGY
Perhaps the most significant shift optomap has enabled is in the quality of communication between primary and secondary eye care. Historically, referral letters described clinical findings in words – findings that could be ambiguous, difficult to locate, or lost in translation at the slit lamp. The ability to transmit optomap images alongside a referral changes that dynamic entirely.
“Whereas previously an optometrist would describe examination findings and sometimes it would be difficult to find them at the slit lamp – now they can communicate with the imaging as well. That’s been really useful,” he said.
The conversation flows in both directions, too. After review, Dr Heydon can send annotated images back to the referring optometrist – confirming a choroidal naevus, for example, with clear documentation of what to monitor and over what timeframe. This creates a visual record that anchors the shared-care relationship in objective evidence rather than descriptive approximation.
The same efficiency extends to specialist-to-specialist collaboration. Dr Heydon recalled a patient seen with a large horseshoe tear. After performing barrier laser, he captured post-treatment optomap images and sent them directly to a vitreoretinal colleague. “Within five minutes, he said he thought it needed some extra treatment, and the patient was booked for cryotherapy the next day to prevent a retinal detachment. It was extremely useful.”
PUTTING PATIENTS IN THE PICTURE
Beyond clinical efficiency and professional communication, Dr Heydon said optomap helps patients understand their own conditions. The vivid, high-resolution images – particularly fluorescein angiography – have an immediate impact when shown to patients who have never before seen inside the back of their own eye.
“I’m always surprised how patients immediately comment on how beautiful the images are,” Dr Heydon said. “It’s quite an unusual thing to see into the depths of the back of your eye, and they really engage with those photos. In the consultation, patients can only take on so much information verbally, so it’s very useful to have that visual picture in their mind – the optic nerve, the macula, the retinal blood vessels. That primes them for subsequent consultations and gives them something objective to look at going forward.”
This engagement has measurable consequences for treatment adherence – particularly in chronic conditions such as diabetes, where patients who understand the stakes are more likely to maintain systemic control. Showing a patient their own retinopathy, explaining what they are seeing, and tracking change over time creates a shared investment in the outcome.
“Once they’ve had treatment – with laser or surgery – we can show them the images and they can see how their eye and vision have responded,” Dr Heydon explained. “That closes the loop for the patient in a way that verbal explanation simply cannot.”
A MODERN STANDARD FOR MEDICAL RETINA
In a field where disease can progress quietly at the edges of the visible retina, and where management decisions depend on accurate staging, objective documentation, and timely communication, Dr Heydon believes that ultra-widefield imaging is rapidly becoming indispensable.
“I think it’s essential in a modern medical retina practice to document baseline findings and severity,” he said. “And having an objective measure with an ultra-widefield system – that’s crucial for making decisions over time, especially in busy clinics where different doctors may be seeing patients across visits.”
“I think it’s essential in a modern medical retina practice to document baseline findings and severity”
As co-management models between optometry and ophthalmology continue to mature across Australia, he said optomap is no longer simply an imaging device – it is the common language through which a modern, collaborative retinal care team speaks.
Dr Heydon did not receive a fee for this interview. Production of this article was sponsored by Optos.

Dr Peter Heydon.