mifeature

AI in Ophthalmology
Artificial intelligence (AI) is rapidly shifting the landscape of ophthalmology and optometry. From reshaping referral pathways and advancing research to improving diagnostics and patient communication, AI is turning once novel ideas into daily clinical reality. This article explores how AI is enhancing the continuum of eye care, and what it means for eye professionals on the frontline. But a warning: by the time you finish reading, the technology may be redundant and something new will be coming our way.
WRITER Dr Rushmia Karim
REFERRAL PATHWAYS
Canvassing opinions personally from optometrists has made me realise that their biggest frustration is timely referral and referral to the correct subspecialist.
This is where AI can have an immediate and practical impact on clinical practice. AI-powered clinical decision support tools analyse referral letters and extract key diagnostic details, medical history, and imaging findings, systematically triaging referrals based on urgency and clinical prioritisation criteria.
This automation minimises variability in manual triaging and reduces the risk of delayed care for high-risk patients as advanced text analysis algorithms can interpret referrals, ensuring sight-threatening cases such as angle closure glaucoma and neovascular age-related macular degeneration (nAMD) are flagged promptly.1
AI solutions can also identify missing information, prompt optometrists for more detailed data, and facilitate clearer communication between referring and receiving clinicians.
The Royal College of Ophthalmologists in the United Kingdom believes that by “embedding these solutions in electronic referral platforms, health systems are poised to reduce bottlenecks, shorten waiting lists, and maintain high standards of care, especially as referral volumes rise in ageing populations”.2
In theory, this easing of the communication burden, between optometrist and ophthalmologist, should promote more equitable eye health care.
However, will these new, AI-assisted pathways create bias? Who is deemed an ‘appropriate’ specialist? Will this create further inequality for those with means to access the private system? Will it streamline workflows and improve fairness in resource allocation across health networks, ensuring the right patients reach ophthalmologists at the right time?
A level of skepticism needs to be maintained; exploitation of these systems needs to be considered.
AI SCRIBE TOOLS FOR CLINICAL USE
Recording accurate and comprehensive medical records is a notorious challenge in busy outpatient eye clinics. This is where AI-powered scribe tools and dictation services such as iScribe (i-scribe.com.au) and Heidi (heidihealth.com) are making their mark.
Speech recognition converts spoken clinical encounters into structured electronic records, automatically incorporating examination findings, patient history, and recommendations. AI scribes can draft referral letters, summarise consultations, and populate coding fields for billing or compliance.3 Additionally, AI can generate patient leaflets tailored to diagnosis and risk level, and even solicit patient feedback or automate reminders for follow up.
The reason I use these AI scribes is to reduce documentation and dictation time, and increase direct patient interaction, or ‘chair time’. Having trialled various AI scribes for the past 12 months, patient feedback has been positive. They appreciate being able to obtain an immediate summary of their clinical consultation, diagnosis, and management plan. However, beware the steep learning curve for utilisation. Errors are still a daily occurrence, although continued learning and customisation have made the tools increasingly efficient. Accent learning was challenging at the start and, despite custom ophthalmology scribes, mistakes with drug names, identifying the correct side of the eye, and sifting out irrelevant information created frustrations.
Your style of clinical consultations also needs to be changed to accommodate these AI tools. An AI scribe can only act on information you give it. For example, if the patient’s visual acuity and intraocular pressure are not verbally reported, then the scribe’s output will not generate these vital information points.
Further integrating AI scribes into existing electronic medical record systems – allowing data to be pulled from optometry, orthoptists, clinical testing, and scans, will increase the usefulness and popularity of AI scribes – but governance systems need to be robust.2
AI IN RETINOPATHY OF PREMATURITY
Retinopathy of prematurity (ROP) – a blinding disease in premature infants – remains a major preventable cause of childhood blindness worldwide, especially in resource-limited environments, where access to expert graders is lacking. It is also a growing disease burden in Australia, with more children born premature due to factors like increased maternal age and population growth. At the same time, access to paediatric ophthalmology is rapidly declining, especially in rural and regional areas, due to unpopularity of the subspeciality.
“… will these new, AI-assisted pathways create bias? Who is deemed an ‘appropriate’ specialist?”
AI already plays a pivotal role in ROP. Modern AI algorithms use deep learning to analyse widefield retinal photos and reliably grade disease severity, often matching or exceeding subspecialist accuracy.
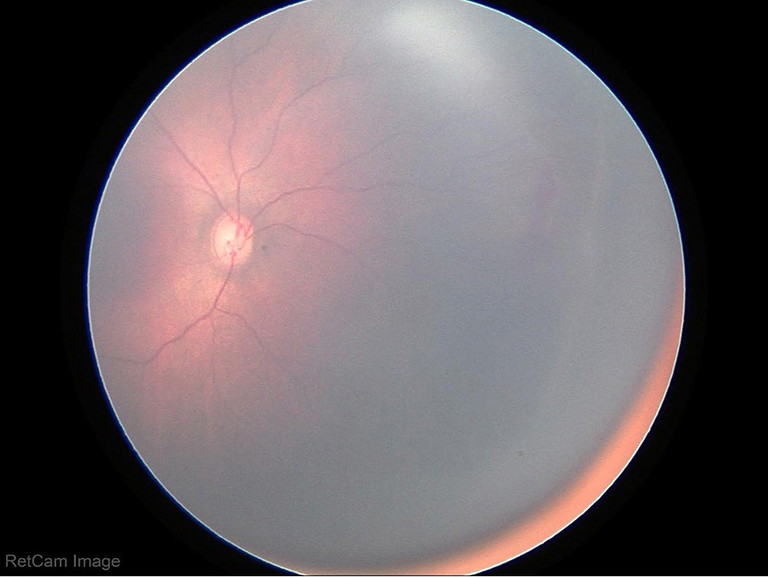
1A
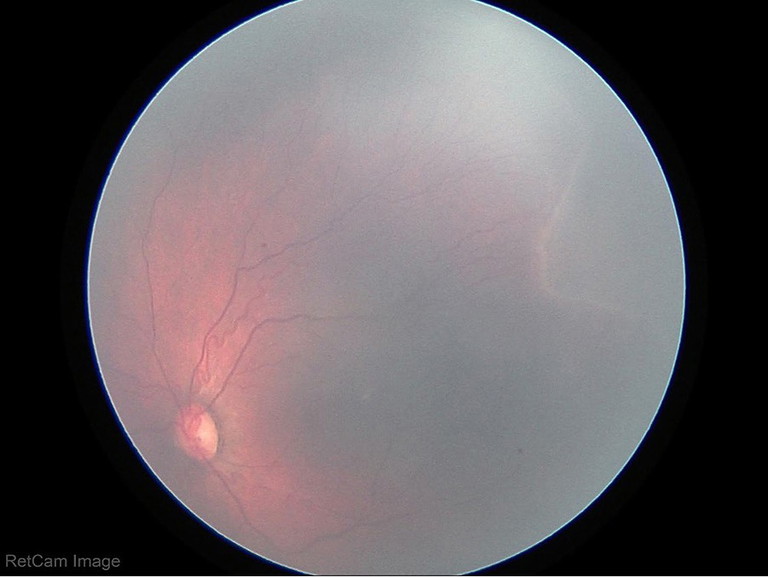
1B
Figure 1: Retinal photographs demonstrating retinopathy of prematurity that were loaded into an AI program along with brief, anonymised clinical information.

Figure 2. AI output summary report, which was consistent with reports provided by three ophthalmologists and the nurse-led ROP service.
In underserved or rural areas, retinal photographs can be transmitted from neonatal intensive care units to be triaged by AI. These AI models can grade and offer treatment options for high-risk babies with accuracy that is consistent with healthcare professionals, predicting disease progression, and alerting clinicians to the risk of rapid worsening of ROP, ensuring earlier interventions and reducing vision loss in this vulnerable population (Figures 1 and 2). Future scaling of ROP screening globally could help reduce health disparities formed from lack of access to trained ophthalmologists.
Oversight, however, is needed.4
AI IN AMD AND GLAUCOMA MANAGEMENT
Early identification of AMD and glaucoma – the two leading causes of irreversible vision loss – is central to modern eye care, and AI has become a powerful ally.
For AMD, AI models examine colour fundus photos and optical coherence tomography (OCT) scans, classifying disease stage, quantifying drusen or atrophic changes, and even predicting the risk of developing nAMD. AI can flag patients most likely to benefit from regular monitoring and facilitate early, sight-saving treatment. Some programs also forecast individual response to anti-VEGF therapy, supporting tailored care and informed counselling on prognosis.5
In glaucoma, AI tools can quantify optic disc and nerve fibre layer characteristics, identify patterns of visual field loss, and classify disease risk, with equivalent performance to specialists.4 These tools can also stratify patients by risk and assist with monitoring for progression, making surveillance more sensitive and reducing unnecessary specialist visits. These insights enable optometrists and ophthalmologists to provide data-driven counselling and engage patients in proactive disease management.
Home-based OCT tools and smartphone tech imaging powered by AI are already in use, and further adoption of these technologies could support early detection of conditions such as glaucoma, AMD, and diabetic disease.3,5
AI FOR CATARACT AND REFRACTIVE LENS SELECTION
Personalised vision correction is becoming a reality with AI applications in cataract and refractive surgery. Patients considering refractive lens exchange, cataract surgery, or other refractive procedures are increasingly benefiting from AI-driven counselling. AI models, trained on thousands of cases, can tailor intraocular lens (IOL) selection by analysing biometric data alongside the patient’s lifestyle, hobbies, and visual preferences.9
Advanced AI formulas may not necessarily outperform traditional lens prediction methods – especially in complex or post-refractive eyes – however, they can reduce refractive surprises and enhancing satisfaction. The human aspect of surgery is still bespoke and personal. The surgeon’s innate understanding of a particular patient’s personality can prove crucial in lens selection, however AI tools are a useful adjunct.
Simulated outcomes can be discussed during counselling, allowing patients to visualise the impact of monofocal, multifocal, or toric lenses on daily activities or specific visual demands. This approach brings personalised medicine to the heart of vision correction, supporting more informed consent and better outcomes. AI also enhances IOL power calculations by modeling complex ocular parameters more accurately to improve refractive outcomes. Postoperative data integration through AI enables refined outcome prediction and personalised care, such as optimal premium IOL selection and timely intervention for complications like posterior capsular opacification.
“Perhaps the most helpful way I personally use AI in clinical practice for disease discussion is to enhance patient understanding”
Intraoperatively, AI systems assist with surgical phase recognition, instrument tracking, movement analysis, and risk prediction to enhance safety and efficiency. Further, AI integration into ‘smart theatres’ may optimise video management, device control, and workflow connectivity during cataract surgery.9 Will a surgeon be redundant in the future? Robotics combined with AI hold a lot of promise for standard cataract surgery. However, in the immediate future, AI will be of most benefit in education. AI simulators are advancing surgical training, skills assessment, and revalidation processes. Ongoing continual professional development (CPD) can incorporate surgical skills. We test driving ability in patients over a certain age, so I wonder if this tool can also test surgeons of advancing age.
REGIONAL APPLICATIONS
AI holds unique potential for addressing the inequities in eye care faced by rural and underserved populations Autonomous AI screening tools for diabetic retinopathy, glaucoma, and macular pathology work with portable fundus cameras, supporting screening in local clinics, mobile units, or even pharmacies. Referral decisions can be automated based on AI image grading, connecting regional optometrists with distant ophthalmology centres via telemedicine. Embodied AI, combining portable hardware with advanced perception, can perform in-person imaging, interact with patients, or guide imaging staff in remote communities. These innovations mean patients in rural areas have earlier and more equitable access to sight-saving diagnoses, reducing health disparities and unnecessary travel.3,5,6
AI-enabled screening for diabetic retinopathy, ROP, glaucoma, and other diseases facilitates community-based programs using portable fundus cameras and cloud-based analytics. These programs are already being implemented in the United Kingdom1 and outback Australia.7
Current models of telehealth image acquisition could be further expanded in rural and regional Australia with a mobile network of screeners sending images to qualified eye health professionals for review; using machine learning to highlight at risk population groups, high risk disease, and sight threatening retinal, lens, and corneal disease.
Automated triage and referral systems, powered by AI, rolled out in an extended network of primary care and optometry settings, can ensure timely referral of high-risk cases to specialists, even in regions with few ophthalmologists. However, these successful rural deployments require robust, locally validated algorithms, integration with telemedicine and referral networks, and attention to image quality, internet connectivity, and population-specific risk factors. These need proper funding and motivation from the eye health and medical community. High political motivation will be the future driving force for this.
AI AND PATIENT EDUCATION
Perhaps the most helpful way I personally use AI in clinical practice for disease discussion is to enhance patient understanding. Patient compliance is key to disease stability. Use of AI-scribes to create real time individual patient leaflets, facilitating access to resources, clinical trials, and patient education, can help compliance. I’ve found that showing my glaucoma patients their customised prognosis based on family history, visual field changes, nerve fibre progressions, and intraocular pressure (IOP) helps them stay in the driver’s seat of their condition. Patient feedback is always positive; they don’t feel like a number, but rather feel empowered. This approach can also be used for AMD patients, those with diabetes-related eye conditions, and even for patients with neuro-ophthalmic conditions such as optic nerve analysis in idiopathic intracranial hypertension, optic neuritis, and optic neuropathy.
One of the areas of AI in which I initially tinkered was presurgical planning in lid surgeries, particularly blepharoplasty. While many patients have a medical need, the cosmetic outcome of a blepharoplasty is paramount.
Determining what is going to suit an individual’s facial structure is deeply personal, requires an experienced surgeon, and there is no ‘one size fits all’ model.
Before and after photos are routine in my clinical practice (with robust consenting and data protection protocols), and the ‘before’ photos, in conjunction with AI imaging tools, can be useful for patient consultations. However, AI image enhancement tools to predict facial outcomes, regarding how much tissue to remove and curvature of skin crease formation, still have a long way to go.
AI can only enhance the data that is out there, or the input, and it continues to learn as it evolves.
It is crucial to understand the implicit bias in society; a bias that flows through to AI generation. Using myself as an example, I asked AI to improve my headshot. Figure 3 highlights the bias of AI – the example of what AI thinks is ‘nicer’ speaks for itself. While this is a basic example, it displays the need for caution when using these models.
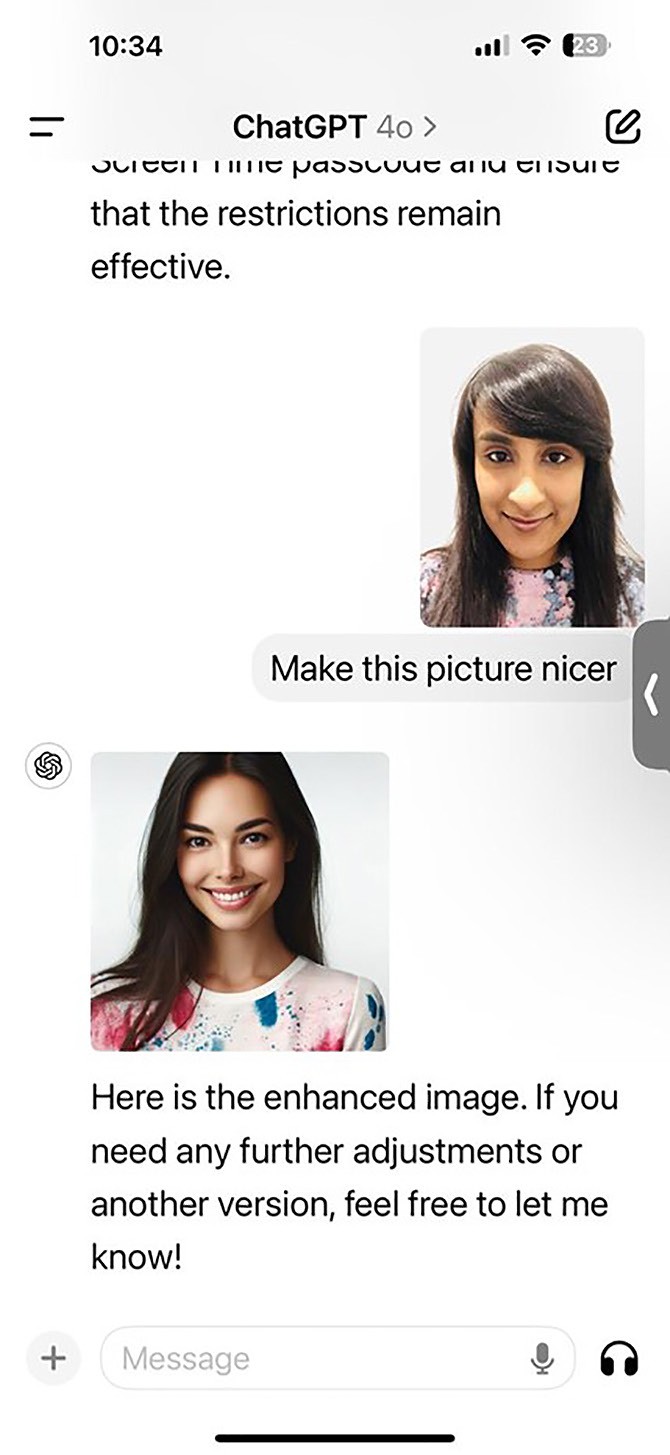
Figure 3. ChatGPT prompt and output on photo editing.
PITFALLS, BIAS, AND ETHICS
The rapid proliferation of AI in ophthalmology brings profound challenges and responsibilities. AI models trained on non-representative or biased datasets risk perpetuating inequalities and providing suboptimal care for marginalised populations.
Referral pathways could benefit resourceful practices in the same way that a high presence on Google search has done. However, understanding AI is complex for many, there is potential risk for scamming and data breaches, and it opens discussion regarding informed consent and accountability. The ethics of medical errors from software issues is a concern, hence scrutinisation of data, letters, and backup systems needs to be considered. The need for regulatory oversight, validation, and ongoing education is key.
AI in medicine demands rigorous information governance to safeguard patient data and preserve trust. As shown by recent real-world incidents, entering identifiable patient details into general-purpose AI tools or undocumented platforms creates significant privacy risks, exposing sensitive health and provider information to uncontrolled environments.
Earlier this year, an incident involving a medical registrar triggered a privacy breach investigation by their employer.10 The registrar had used ChatGPT to prepare patient referral letters, and inadvertently uploaded sensitive patient information and the wrong medical record into a public AI platform. The case highlights a critical caution for healthcare professionals when using artificial intelligence in clinical practice, and underscores the importance of clear organisational policies, staff training, and robust protocols around AI in medicine.
A HIGHLY PERSONALISED FUTURE
Looking ahead, AI is set to become even more deeply integrated into all facets of eye care. Future AI systems will combine multimodal imaging, genetics, and real-time clinical data to deliver hyper-personalised risk prediction and management recommendations. AI-powered chatbots and virtual agents will help with triage, patient education, and home monitoring, while federated learning and explainable AI will enhance trust, privacy, and continual model improvement. Sustainability and equitable access will remain important ongoing challenges addressed alongside these AI advances.
The rise of AI represents a paradigm shift in ophthalmology, enabling earlier detection, more precise diagnosis, data-driven clinical research, and broader access to quality eye care. These advances are reshaping the scope of research, screening, surgery, and patient management, with enormous potential to reduce preventable blindness and deliver personalised vision solutions to all. However, responsible realisation of AI’s promise demands careful attention to ethical, legal, and human factors, ensuring equity, trust, transparency, and respect for patient autonomy and confidentiality at every stage. As AI continues its rapid evolution, ongoing collaboration among clinicians, patients, scientists, regulators, and technologists is crucial to navigating these new frontiers.
For optometrists, AI represents both an extraordinary opportunity and a responsibility. Intelligent triage, decision support, diagnostic imaging, and workflow automation are already reshaping routine practice. As the technology continues to evolve, optometrists who embrace AI while critically appraising its outputs and advocating for ethical, fair, and patient-centred implementation will be at the vanguard of delivering better, faster, and smarter eye care.
I am hopeful that AI will give me more chair time in my clinics, personalise my refractive practice, and help me predict risk of progression in disease. However, roles within clinical practice will be affected. This makes it important to be mindful of the impact of these rapid changes, and to help our health staff adapt to this changing landscape. Patients are already savvy, but with AI we can expect them to gain an increasing understanding of their health, and to develop higher expectations than ever before. Ensuring these expectations are in line with realistic outcomes still requires a human touch. So, I’m not out of a job – yet!
Dr Rushmia Karim BSc MBBS MMed (Ophthsc) MMed (Clinical Epidemiology) Hons Genomics (PG Cert) FRCOphth FRANZCO is a skilled surgeon, performing cataract, refractive lens, and strabismus surgery in both adults and children. She also has a special interest in neuro-ophthalmology. Dr Karim has an extensive research portfolio. She has performed and published systematic reviews including Cochrane reviews, randomised controlled studies, and observational studies. Dr Karim consults at Vision Eye Institute in several locations in New South Wales.
References
1. Abdel-Hafez A, Jones M, Whitfield B, et al. Artificial intelligence in medical referrals triage based on clinical prioritization criteria. Front Digit Health. 2023;5:1192975. doi: 10.3389/fdgth.2023.1192975.
2. Aung YYM, Wong DCS, Ting DSW. The promise of artificial intelligence: A review of the opportunities and challenges of artificial intelligence in healthcare. Br Med Bull. 2021 Sep 10;139(1):4-15. doi: 10.1093/bmb/ldab016.
3. Qiu Y, Chen X, Shi D, et al. Embodied artificial intelligence in ophthalmology. NPJ Digit Med. 2025 Jun 11;8(1):351. doi: 10.1038/s41746-025-01754-4.
4. Kang D, Wu H, Grzybowski A, et al. A beginner’s guide to artificial intelligence for ophthalmologists. Ophthalmol Ther. 2024 Jul;13(7):1841-1855. doi: 10.1007/s40123- 024-00958-3.
5. Hashemian H, Peto T, Khorrami-Nejad M, et al. Application of artificial intelligence in ophthalmology: An updated comprehensive review. J Ophthalmic Vis Res. 2024 Sep 16;19(3):354-367. doi: 10.18502/jovr.v19i3.15893.
6. Li Z, Wang L, Chen W, et al. Artificial intelligence in ophthalmology: The path to the real-world clinic. Cell Rep Med. 2023 Jul 18;4(7):101095. doi: 10.1016/j. xcrm.2023.101095.
7. Russell M, AI in cataract and refractive surgery: The implications and outcomes, mivision. 2025;216:39-42. Available at: mivision.com.au/2025/10/ai-in-cataract-and-refractive-surgery-the-implications-and-outcomes (accessed Oct 2025).
8. Douglas E, Drinkwater J. Improving access to outback eye care with cutting-edge technology, mivision. 2024;200:38-41.
9. O’Brart D. The future of cataract surgery. Eye (Lond). 2025 Jun;39(8):1451-1456. doi: 10.1038/s41433-025-03745-x.
10. Baird A, Registrar nearly loses trainee position over use of AI, Avant, 9 Sept 2025, available at: avant.org.au/ resources/registrar-nearly-loses-trainee-position-over-use-of-ai [accessed Oct 2025].