mieducation

BCLA CLEAR Presbyopia
Management with Corneal Techniques
In this final article from a series that captures the clinically relevant conclusions from the BCLA CLEAR Presbyopia publications, Dr Neema Ghorbani-Mojarrad and Professor Jennifer Craig provide an overview of corneal management approaches for presbyopia.
WRITERS Dr Neema Ghorbani-Mojarrad and Professor Jennifer Craig
LEARNING OBJECTIVES
On completion of this CPD activity, participants should:
1. Be able to advise patients on temporary and permanent options for presbyopia correction via corneal alterations,
2. Realise the importance of careful patient selection and education,
3. Understand the optometrist’s role in managing patient expectations from surgery, and
4. Understand the optometrist’s role, pre and post surgery, to optimise visual outcomes.
This article explores the correction of presbyopia through temporary and permanent corneal alterations, drawing on insights from the British Contact Lens Association (BCLA) CLEAR publication on the management of presbyopia with corneal techniques. There are two reasons for why this is important for eye care practitioners. First, if we encounter a patient who has previously undergone these treatments, we need to be aware of what has occurred and the key points to consider when managing the patient in our clinic. Second, we need to be prepared for a patient enquiring about options for presbyopia correction beyond our traditional optical device means. We need the knowledge to advise and discuss alternative options comprehensively and effectively.
PRE-TREATMENT PATIENT SELECTION
According to best practice, a comprehensive pre-treatment or assessment plan is needed when consulting patients about surgical corneal interventions. This is particularly important because many of these interventions are intended to be permanent. Discussion is required to ensure that expectations for resulting visual outcomes are appropriately managed. Patient selection is imperative; it is important that ahead of any corneal intervention a comprehensive history is taken to ensure the patient is suitable for any proposed approach, and that any prior treatments (whether successful or not) are recorded. Any history of unstable refraction, corneal abnormality (particularly corneal ectasias such as keratoconus), uncontrolled external eye disease, or systemic condition that may impact surgical healing or underlying disease such as diabetes or immune-related disease, is a potential contraindication, and therefore should be screened for.1 Full evaluation of ocular health is required; patients with glaucoma may not be suitable for a number of the treatments due to the increased intraocular pressure that occurs during surgery, and a thorough assessment of retinal and crystalline lens health is required.
Additionally, it is important that patients who are chosen for irreversible corneal interventions are not promised unachievable outcomes. Patients with greater visual demands and requirements for high levels of stereoacuity or contrast detail may not be suitable for corneal treatments with an intended monovision result, or a risk to contrast sensitivity. Age is also an important success factor; early presybopes aged between 45 to 55 are potential candidates for corneal techniques, while older presbyopes may not have as good visual outcomes due to the greater addition power requirement as well as present or impending lenticular changes that may make them better candidates for crystalline lens treatments.2
High patient satisfaction is associated with setting realistic patient expectations prior to surgery.6 However, it is worth noting that presbyopic corneal surgery has a lower rate of patient satisfaction and spectacle independence than surgery to correct vision for a single distance.7 Additionally, there’s a lack of long-term patient satisfaction outcomes for presbyopic corneal correction. One of the longest longitudinal studies showed sustained visual improvement in both distance and near for five years post surgery.8 Other studies looking at patient satisfaction long term have mostly been in pre-presbyopes.9 Therefore, further research exploring perceived benefits beyond the first few years post treatment for different treatments, and specifically in treated presbyopic patients, is recommended. This is particularly important given the progressive nature of presbyopia, which can result in a perceived reduction in efficacy over time.
Corneal surgical techniques all have refractive error limits, which vary depending on treatment type. Some laser interventions now have approval for correction up to -14.00D of myopia (with -6.00D of astigmatism), and +6.00D of hyperopia (with +5.00D of accompanying astigmatism). However, this will depend on patients’ baseline ocular characteristics (e.g., corneal thickness) as well as the type of laser being used. Other treatments, such as corneal inlays, are not intended to adjust distance refraction, and thus have a much narrower distance correction limit (of up to ±1.00D). With regard to near refractive error limits, most have a maximum near correction of +2.00D, but this can vary across different treatments.
Patient Evaluation
Careful evaluation of the anterior eye is vital prior to treatment. Pre-treatment visual acuity and contrast sensitivity are necessary to provide initial measures of visual function, and patients should be aware that no procedure is expected to improve upon the baseline values obtained. Tomography/ topography can be used to evaluate corneal regularity and presence/risk of corneal ectasia. The results can also be applied in the customisation of some surgical procedures, such as those used to reduce corneal astigmatism.3 Similarly, assessing aberrometry can provide an estimate of pre-treatment status and may offer the opportunity for further corneal customisation to enhance post-operative visual quality.4 Evaluating entrance pupil size is also important for most techniques that induce multiple focal points within the cornea, to allow adequate area for different planes of focus. Pupil diameter informs some surgical treatment selection, particularly for wavefront-guided procedures, to maximise the treatment zone.5
Adverse Outcome Assessment
Assessments are also performed to determine the risk of adverse outcomes. One of the most feared complications is that of surgically-induced corneal ectasia, as this can cause irreversible visual impairment. The current rate of occurrence is between 0.03–0.66% of all treated eyes.11 In light of this, several scoring systems have been established to help identify eyes at risk. These include the ectasia risk scoring system (ERSS) and the percentage tissue altered.11,12
With the ERSS in Table 1, each risk factor is given a score from 0 to 4, with a score of 0 indicating minimal or no risk, and a score of 4 indicating the highest risk. A cumulative score from all factors of between 0 and 2 indicates low risk to the eyes, and scores of 4 or higher indicate greater risk, for which treatment may be avoided. The percentage tissue altered system works with the underlying principle that the more tissue that is altered, the greater the risk, and a value exceeding 40% alteration of the corneal tissue is considered the threshold for greater risk. Practitioners have been advised that using a combination of both of these two approaches allows for a more holistic assessment of risk for each patient.
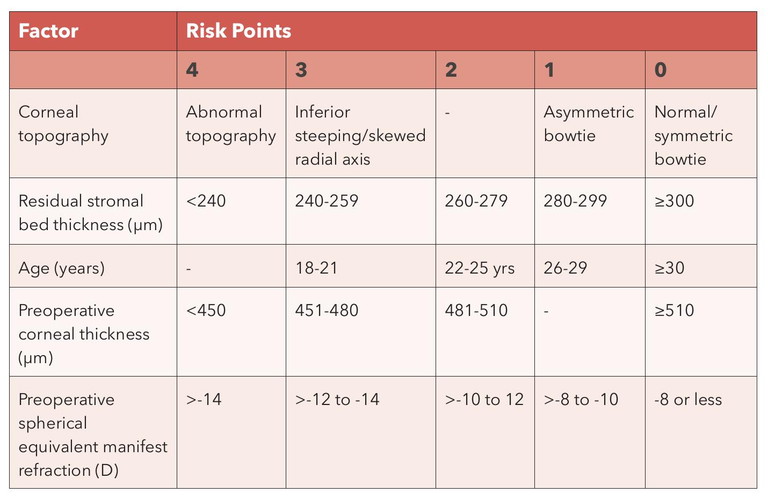
Table 1. The Ectasia Risk Score System. Note that there is no consideration of recent refractive change, which may also be an indicator of risk.
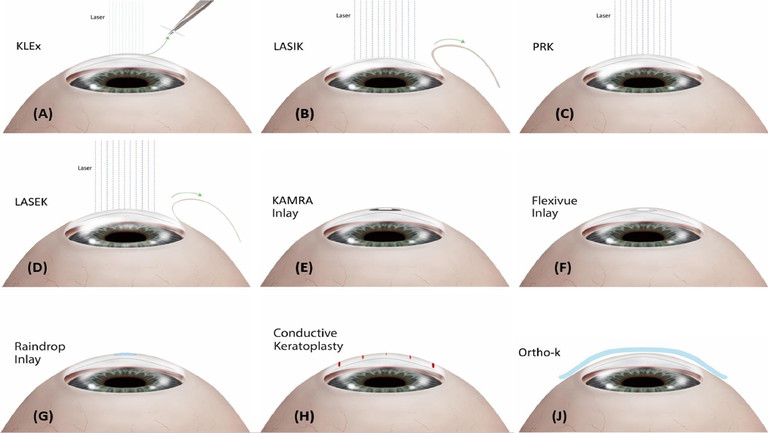
Figure 1. Permanent surgical corneal interventions for presbyopia.
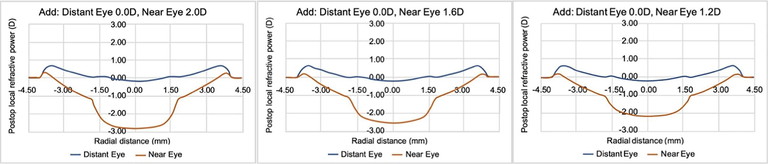
Figure 2. Power profiles of the cornea with a residual defocus of -0.89D in the near eye. From left to right, the addition is reduced from 2.0D to 1.6D to 1.2D in the near eye. Reprinted with permission from BCLA CLEAR Presbyopia: Management with corneal techniques.
CORNEAL TREATMENT OPTIONS
Reversible corneal treatment options: Although orthokeratology cannot be excluded as an option for presbyopia correction, it typically offers only a monofocal refractive change. This allows for monovision correction (one eye corrected for distant vision, one for near). This is relatively rare in clinical practice, and due to the availability of other contact lens presbyopia correction options, which are more accessible, this mode of correction is not discussed further in this article.
Permanent corneal treatment options: Broadly speaking, surgical corneal interventions for presbyopia can be divided into three categories: laser refractive correction, corneal inlays, and conductive keratoplasty (Figure 1).
Corneal Laser Surgery
Similar to contact lenses that have monovision and multifocal presbyopia correction options, corneal laser surgery for presbyopia follows the same two principles.
Monovision laser-assisted in-situ keratomileusis (LASIK) correction was approved by the United States Food and Drug Administration (FDA) in 2007, and was the initial approach of choice in corneal presbyopia correction. There are some reports that patient satisfaction with this approach was as high as 98%, which would exceed that typically seen with monovision contact lens correction of presbyopia. However, data unsurprisingly demonstrate a slight decrease in contrast sensitivity and stereopsis following treatment. Some new approaches to overcome this are to use the laser to create different shape alterations, with the aim of increasing the range of focus in treated eyes by inducing higher order aberrations, or with tailor-made approaches to counteract corneal aberrations, such as spherical aberration. These have been shown to improve outcomes, but with variable success depending on the study and the correction strategy selected.
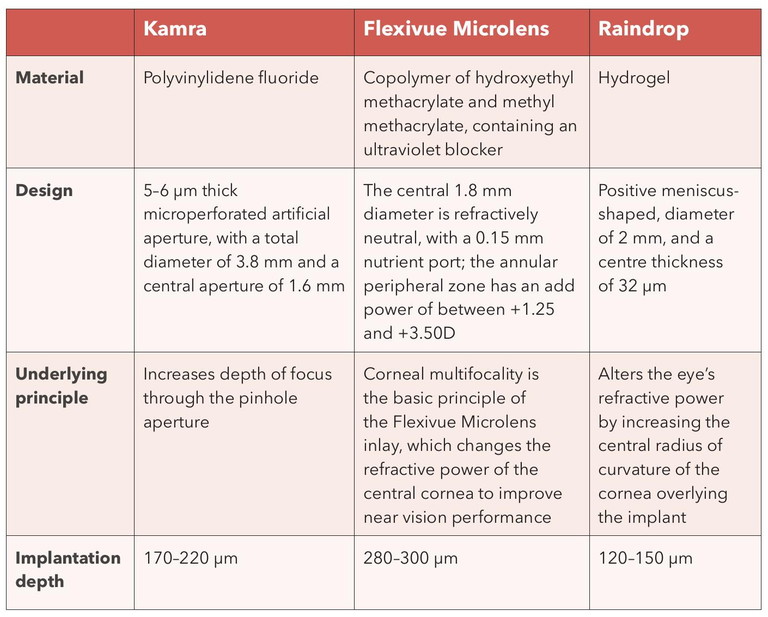
Table 2. Comparison of three intracorneal inlays, discussing their material, design, and method of correction. As shown in BCLA CLEAR Presbyopia: Management with corneal techniques.
Interestingly, a retrospective study of 284 LASIK patients over the age of 45 demonstrated that 188 had opted for monovision and that while most chose their dominant eye for distance vision (85%), those that did not experienced a similar level of visual outcome and overall satisfaction.12 Nevertheless, 35% of those who initially opted for monovision subsequently chose to have further treatment to remove the monovision, with 7% requesting correction of their near eye for distance vision, and 28% requesting further enhancement of their distance eye. Therefore, generally, it appears that monovision corneal LASIK does show favourable outcomes, likely supported by the prerequisite for patients to demonstrate a successful monovision trial with contact lenses before committing to more permanent surgery.
For multifocal corneal treatments (also known as multifocal LASIK or PresbyLASIK), once again, the general concept of the corneal treatment is similar to that of contact lenses, with either multifocal designs, or with some adjustment for distance and near eyes with a hybrid/modified monovision-type approach.
This might include treatment in a multifocal manner for a single eye, such as PresbyMax, which corrects one eye for distance vision, and the contralateral eye for increased range of focus at near using a multifocal correction. Generally, the treatment is based on the creation of a positively powered corneal zone centrally for near vision, with the pericentral and peripheral cornea treated for distance vision (i.e., centre-near design). Some central areas have been shown to allow a similar focussing ability to that of a +2.00D near addition, and have shown generally good satisfaction levels. Similar to that of contact lens designs, multifocal corneal surgery relies on pupil size changes to allow for simultaneous perception, focussing on near with the central cornea. Patient selection based on good pupil responses and range is therefore required to minimise the risk of patient dissatisfaction. Figure 2 gives an example of the power profile of the cornea of a presbyopic multifocal correction, across a range of different near addition powers, in the near vision eye. Although a range of surgical power profiles and ablation designs are available, it is worth noting that some surgeons will give prospective patients a multifocal contact lens trial of various powers to help assess patient adaptability and determine whether a particular addition power may work best for a patient in their day-to-day tasks. Such trials are well suited to being performed in collaboration with optometrists to enable patients to make informed decisions, should they wish to consider this approach. Nonetheless, more research looking at the various approaches and designs for their long-term patient satisfaction would be highly beneficial.
Corneal Inlays
Corneal inlays are primarily designed for emmetropic patients with little or no distance prescription. The inlays are surgically inserted between lamellae of the cornea, at different depths within the stroma. They improve near vision by adjusting the way that light rays enter the eye, to facilitate near focus.
Three intracorneal inlays were discussed in the report. These are shown in Table 2. They have different mechanisms of action, for example the Kamra inlay, which was first approved in 2015, increases depth of focus using a pinhole approach to facilitate viewing at near, and the other two inlays function by altering the refractive power and radius of curvature of the cornea around the implant to improve near vision.
Reported outcomes with these inlays have been generally positive, with a systematic review finding that nearly 91% of patient eyes had a distance vision of 6/7.5 or better, and 79% obtained a near vision of N4/N5 or better.14 Results from other inlays and studies of implants have similarly shown positive outcomes, however patient satisfaction is difficult to compare across studies, due to the lack of validated patient-reported outcome measures being used. Longer-term studies are vital in evaluating these newer technologies; for example while the Raindrop implant received excellent initial outcomes, it was ultimately withdrawn from the market due to 42% of patients exhibiting corneal haze after five years.15
In addition to this, there have been reports that some patients may experience changes in refraction after surgery. There have been reported reductions in contrast sensitivity, increased corneal aberrations, and adverse events related to the materials used, such as corneal necrosis and melt, and scar tissue formation. In light of this, allogeneic inlays have been made, such as the PrEsbyopic Allogenic Refractive Lenticule (PEARL) inlay. Over a six-month follow-up period, no safety concerns were demonstrated, and these findings were echoed in a 12-month case series of patients and a three-year unilateral study of 25 patients, using their non-dominant eye. Further work, however, is required to observe patient outcomes beyond three years, and in greater patient numbers.
Conductive Keratoplasty
Conductive keratoplasty (CK) is a noninvasive procedure in which radio frequency energy (at 350–400kHz) is applied to the mid-periphery of the cornea to treat mild to moderate hyperopia (up to +3.00D) and presbyopia. The procedure is performed using a small device with a sterile probe that applies radio energy to heat the collagen of the stroma to about 65°C, creating tiny, U- or V-shaped marks. These marks are arranged in a ring pattern, usually around 8, 16, 24, or 32 spots, depending on the magnitude of correction needed. More spots equate to stronger correction and, for presbyopia, this is primarily achieved by applying differential amounts of treatment to the two eyes, aiming to provide one eye with more positive power in a monovisionlike approach (although attempted multifocality has been reported).16 Typically, the treatment is applied only to one eye – usually the non-dominant eye – to improve near vision.
“Beyond the initial post-surgical follow-up period, there remains a need for lifelong optometric care”
Visual outcomes have generally been positive, with about 89% of eyes achieving distant vision of 6/7.5 or better after 30 months, and an N5 equivalent at near. Some studies have reported an increase in corneal astigmatism after treatment, but studies evaluating contrast sensitivity have reported no clinically significant differences after treatment, although data is limited. Multicentre clinical trials demonstrate good success in patients, with 63% of patients achieving outcomes within half a dioptre of emmetropia in the distant eye. However, this was in pre-presbyopic patients, and the studies have demonstrated that over time, there is regression and that the effects of treatment can diminish after 24 months.18 Despite this, patient satisfaction and visual improvement after treatment have been reported to be high, even after 24 months.
POSTOPERATIVE MANAGEMENT
Postoperative care is important and will vary according to procedure. Intensive follow-up is typically recommended over the first 48–96 hours immediately following surgery, with follow-up continuing for a minimum period of three months to provide sufficient stabilisation time for corneal tissues and refraction. Beyond the initial post-surgical follow-up period, there remains a need for lifelong optometric care.
Typical patient complaints initially after treatment can relate to discomfort and foreign body sensation, visual disturbance, and symptoms related to the adjunctive postoperative therapies (such as antibiotic or anti-inflammatory eye drops). After the initial healing and stabilisation, care should be focussed on optimising quality of life, visual ability, and overall satisfaction.
Patients require functional and structural evaluation of the eyes, which includes tests typically performed within a sight test and anterior eye assessment, to examine the cornea, conjunctiva, limbus, lids and lashes, and overall ocular adnexa. Additional tests, such as corneal topography/tomography, pachymetry, and contrast sensitivity, are also strongly recommended, as well as assessment of corneal endothelial cell density, if possible.
Longer Term Effects
Patients can have adverses effects that may impact them over the long term. Neuropathic pain can occur due to adverse effects on the innervation of the cornea, and can present as symptoms of burning, stinging, or severe dryness that appears out of proportion to observable corneal signs. A systematic review of the impact of refractive surgery on corneal nerves found that greater depths and diameters of corneal ablation, flap size, and magnitude of original refractive error were associated with increased effects on corneal nerves and sensitivity.17 The nerves are expected to heal, although not necessarily fully, with 10-year post-LASIK confocal microscopy measures on post-surgery patients demonstrating reduced nerve density compared to controls.19
Dry eye is also a common feature in many patients, particularly for those with presbyopia, due to increased age which is an inherent risk factor for both conditions. However, the risk of dry eye post-surgery is greater in patients with higher pre-surgery refractive error and greater ablation depth, as well as in females, prior contact lens wearers, and those of South Asian ethnicity. LASIK surgery can lead to a marked decrease in tear production and stability compared to patient baseline, and thus pre-emptive assessment and management of dryness signs and symptoms, both before and after surgery, can be beneficial.
Dysphotopsia can also occur following surgery, reported as starbursts, haloes, glare, or image degradation. Similar to other adverse effects, factors associated with an increased risk are higher refractive error and greater ablation depth treated. Smaller diameter treatments and larger pupils are also associated with these adverse effects, as refractive changes near the edges of the treatment zone become noticeable within the pupil area. Re-treatment over a larger ablation zone can decrease haloes, and using miotic agents to reduce the pupil size has also been suggested.
Wavefront-guided ablation can potentially reduce any irregular astigmatism after LASIK surgery.
SUMMARY
Corneal techniques to manage presbyopia involve a range of different approaches, most of which are permanent or semi-permanent. Patients should be carefully assessed for suitability, and a comprehensive examination by a surgeon or their team, alongside careful aftercare, is important to maximise patient satisfaction and success. Corneal laser treatments are often similar in their approaches to those of presbyopic contact lens correction, including both monovision and multifocal modalities, and thus patients considering these treatments are often offered, and benefit from, trialling equivalent contact lens fits to experience how their vision may be and their likelihood of adaptation.
Optometrists should remain informed and up-to-date with the different forms of corneal treatments available for presbyopia, as they can play an important role in helping patients understand their options. Optometrists can also potentially help their patients experience, through contact lens trial, something akin to the visual outcomes achievable with surgery.
Further research into longer-term patient satisfaction and outcomes for these treatments is warranted.
There are several other areas of the BCLA CLEAR Presbyopia Corneal Techniques report beyond the scope of the current article, and interested readers are encouraged to read the full article for a review of other treatments such as orthokeratology for presbyopia, other factors to consider in post-operative care, and future areas and directions for research where further scientific evidence would be beneficial.
Five Key Takeaways
1. Patients considering corneal surgery typically have choices of LASIK, corneal inlays, and conductive keratoplasty.
2. Most corneal techniques use optics similar to monovision or multifocal contact lenses.
3. Patients will usually have a contact lens trial to assess suitability and likely success of surgical intervention.
4. Managing patient expectations is extremely important in both pre-and post-treatment care.
5. More studies looking at long-term (5+ years) follow-ups of presbyopic corrected patients would be beneficial.
To earn your CPD hours from this activity, scan the code or visit mieducation.com/bcla-clear--presbyopia-managementwith-corneal-techniques.
Acknowledgement and recognition to the paper’s authors: Jennifer P Craig, Allon Barsam, Connie Chen, Obinwanne Chukwuemeka Jr, Neema Ghorbani-Mojarrad, Florian Kretz , Langis Michaud , Johnny Moore, Lucia Pelosini, Andrew MJ Turnbull, Stephen J Vincent, Michael TM Wang, Mohammed Ziaei, and James S Wolffsohn.

The paper is open access and available at BCLA CLEAR Presbyopia: Management with corneal techniques in Contact Lens and Anterior Eye (contactlensjournal.com) or via the QR code.
This initiative was facilitated by the BCLA, with financial support by way of educational grants provided by Alcon, Bausch and Lomb, CooperVision, EssilorLuxottica, and Johnson and Johnson Vision. The editors for this article series are Neil Retallic and Dr Debarun Dutta.


Dr Neema Ghorbani-Mojarrad PhD BSc (Hons) MCOptom FBCLA FIACLE Prof Cert Glaucoma and Low Vision Dip SV FHEA is an Associate Professor at the University of Bradford, Chair of the British and Irish University and College Contact Lens Educators (BUCCLE), and a BCLA Fellow and council member.

Professor Jennifer P. Craig BSc (Hons) MSc (Cataract and Refractive Surgery) PhD FCOptom FAAO FBCLA FACLS is a Professor in Ophthalmology at The University of Auckland and a BCLA Fellow and Global Ambassador.
References
1. Jacobs DS, Lee JK, Vitale S, et al; American Academy of Ophthalmology preferred practice pattern refractive management/intervention panel. Refractive surgery preferred practice pattern. Ophthalmology. 2023 Mar;130(3):P61-P135. doi: 10.1016/j.ophtha.2022.10.032.
2. Fernández J, Rodríguez-Vallejo M, Piñero DP, et al. From presbyopia to cataracts: a critical review on dysfunctional lens syndrome. J Ophthalmol. 2018 Jun 27;2018:4318405. doi: 10.1155/2018/4318405.
3. Koller T, Iseli HP, Seiler T, et al. Q-factor customized ablation profile for the correction of myopic astigmatism. J Cataract Refract Surg. 2006 Apr;32(4):584-9. doi: 10.1016/j.jcrs.2006.01.049.
4. Manche E, Roe J. Recent advances in wavefront-guided LASIK. Curr Opin Ophthalmol. 2018 Jul;29(4):286-291. doi: 10.1097/ICU.0000000000000488.
5. Sutton G, Lawless M, Hodge C. Laser in situ keratomileusis in 2012: a review. Clin Exp Optom. 2014 Jan;97(1):18-29. doi: 10.1111/cxo.12075.
6. McGhee CN, Craig JP, Brown AD et al. Functional, psychological, and satisfaction outcomes of laser in situ keratomileusis for high myopia. J Cataract Refract Surg. 2000 Apr;26(4):497-509. doi: 10.1016/s0886-3350(00)00312-6.
7. Moussa K, Jehangir N, Moshirfar M, et al. Corneal refractive procedures for the treatment of presbyopia. Open Ophthalmol J. 2017 Apr 27;11:59-75. doi: 10.2174/1874364101711010059.
8. Moussa K, Jehangir N, Moshirfar M, et al. Corneal refractive procedures for the treatment of presbyopia. Open Ophthalmol J. 2017 Apr 27;11:59-75. doi: 10.2174/1874364101711010059.
9. Luger MHA, McAlinden C, Arba-Mosquera S, et al. Long-term outcomes after LASIK using a hybrid bi-aspheric micro-monovision ablation profile for presbyopia correction. J Refract Surg. 2020 Feb 1;36(2):89-96. doi: 10.3928/1081597X-20200102-01. Erratum in: J Refract Surg. 2024 Jan;40(1):e67. doi: 10.3928/1081597X-20231205-06.
10. Moshirfar M, Tukan AN, Hoopes PC, et al. Ectasia after corneal refractive surgery: A systematic review. Ophthalmol Ther. 2021 Dec;10(4):753-776. doi: 10.1007/s40123-021-00383-w.
11. Randleman JB, Trattler WB, Stulting RD. Validation of the ectasia risk score system for preoperative laser in situ keratomileusis screening. Am J Ophthalmol. 2008 May;145(5):813-8. doi: 10.1016/j.ajo.2007.12.033.
12. Santhiago MR, Smadja D, Randleman JB, et al. Association between the percent tissue altered and post-laser in situ keratomileusis ectasia in eyes with normal preoperative topography. Am J Ophthalmol. 2014 Jul;158(1):87-95.e1. doi: 10.1016/j.ajo.2014.04.002.
13. Braun EH, Lee J, Steinert RF. Monovision in LASIK. Ophthalmology. 2008 Jul;115(7):1196-202. doi: 10.1016/j.ophtha.2007.09.018.
14. Pluma-Jaramago I, Rocha-de-Lossada C, Rachwani-Anil R, Sánchez-González JM. Small-aperture intracorneal inlay implantation in emmetropic presbyopic patients: a systematic review. Eye (Lond). 2022 Sep;36(9):1747-1753. doi: 10.1038/s41433-022-02032-3.
15. Moshirfar M, Desautels JD, Hoopes PC, et al. Comparison of FDA safety and efficacy data for KAMRA and Raindrop corneal inlays. Int J Ophthalmol. 2017 Sep 18;10(9):1446-1451. doi: 10.18240/ijo.2017.09.18.
16. Stahl JE. Conductive keratoplasty for presbyopia: 3-year results. J Refract Surg. 2007 Nov;23(9):905-10. doi: 10.3928/1081-597X-20071101-07.
17. Ehrlich JS, Manche EE. Regression of effect over long-term follow-up of conductive keratoplasty to correct mild to moderate hyperopia. J Cataract Refract Surg. 2009 Sep;35(9):1591-6. doi: 10.1016/j.jcrs.2009.05.010.
18. Campos M, Hertzog L, Garbus JJ, McDonnell PJ. Corneal sensitivity after photorefractive keratectomy. Am J Ophthalmol. 1992 Jul 15;114(1):51-4. doi: 10.1016/s0002-9394(14)77412-4.