mieducation

Protecting the Cornea in Glaucoma:
Why I Intervene Earlier with MIGS
One of the most common things I hear from patients living with glaucoma is not that their vision is deteriorating, nor that their pressures are too high – but that their eyes are sore. Tired, red, gritty, uncomfortable eyes are part of the daily lived experience for many people on long-term topical therapy. For some, this discomfort has become so normalised that they no longer attribute it to their treatment. Yet as clinicians, we notice the keratopathy, lid margin keratinisation, meibomian gland dysfunction, conjunctival hyperaemia, and micropapillary responses that silently accumulate across years of medical management. So what can we do to help these patients?
WRITER Dr Nicholas Toalster
LEARNING OBJECTIVES
On completion of this CPD activity, participants should be able to:
1. Describe mechanisms by which chronic topical glaucoma therapies contribute to ocular surface disease,
2. Explain the role of MIGS in reducing medication burden and improving long term outcomes, and
3. Identify clinical scenarios appropriate for early MIGS referral within collaborative care.
Consider this typical case I managed: a 67-year-old lady with early–moderate open-angle glaucoma, and ‘stable pressures’ in the mid-teens on three different agents. Her visual fields showed mild scattered changes, fluctuating, and perhaps slowly progressing; optical coherence tomography (OCT) showed slow attrition. On paper, this patient was reasonably well controlled. In the chair, however, she told a different story. Her eyes were inflamed with evidence of punctate epithelial erosions, reduced tear film break-up time, congested conjunctiva, fluctuating visual quality, and persistent foreign-body sensation.
The burden these patients carry is not a function of their optic nerve, but of their ocular surface.
This tension between disease stability and treatment toxicity is one of the defining challenges of contemporary glaucoma care. Traditionally, our paradigm prioritised intraocular pressure (IOP) above all else. If the pressure was acceptable and the fields were stable, the therapy was considered successful. But as glaucoma care has stretched across decades, we have become increasingly aware that glaucoma is not a disease of the optic nerve alone. The ocular surface and conjunctiva are also deeply affected by the treatments we choose.
Over the past decade, the emergence of minimally invasive glaucoma surgery (MIGS), in combination with selective laser trabeculoplasty (SLT), has allowed us to rethink what ‘early intervention’ means.
Rather than using more aggressive surgery, early intervention can now represent a lower-morbidity, safer approach that reduces lifelong medication exposure, preserves conjunctival integrity, and protects the ocular surface and cornea. This shift in thinking – away from purely IOP-centric outcomes and toward whole-eye health – has become central to how I counsel and manage my patients.
This article discusses how MIGS has changed my treatment paradigm, why I intervene earlier than I once did, and how protecting the cornea and ocular surface has become a key consideration in glaucoma care.
RETHINKING EARLY INTERVENTION IN GLAUCOMA
For many years, glaucoma management followed a predictable ladder: Start with a single topical medication, add a second, then a third, consider laser. Then, when medications and laser fail, proceed to trabeculectomy or a tube shunt.
This model emerged when drops and filtering surgery were our only real options. Drops were simple and accessible, while surgery was reserved for advanced disease because the risks were significant.
However, several limitations of this ladder have become increasingly clear.
Medication burden is not benign. Long-term topical therapy contributes to ocular surface disease (OSD), with preservative exposure playing a major role. Benzalkonium chloride (BAK) and other preservatives are still common in glaucoma medications and these cause epithelial toxicity, goblet cell loss, inflammation, limbal stem cell stress, and destabilisation of the tear film.1-3Even preservative-free medications can exacerbate OSD through pH changes, osmolarity effects, or active ingredient side effects.
The result is fluctuating vision, photophobia, stinging, burning, foreign-body sensation, and reduced quality of life. Many patients find these symptoms far more bothersome than the glaucoma itself.
Importantly, OSD also contributes to variable visual fields, poor compliance, and increased risk of complications during future filtering surgery. Additionally, compromised conjunctiva is strongly associated with trabeculectomy failure.4 Years of polypharmacy, prior injections, or previous filtration surgery can leave the conjunctiva thin, inflamed, and fibrosed – all factors that complicate subsequent interventions.
Cataract and corneal surgery require a healthy surface. We now all live at a time where patients demand excellent visual outcomes from their glasses, contact lenses, and cataract surgery (and other procedures). Accurate keratometry, reliable biometry, stable tear film, and refractive outcomes all depend on an intact ocular surface. Patients with long-standing OSD from glaucoma therapy have a higher likelihood of fluctuating visual quality, postoperative discomfort, and suboptimal refractive outcomes after cataract surgery.5,6
SLT is useful – but not a complete solution. SLT is an excellent early therapy, and micropulse cyclodiode laser is promising. These avoid the ocular surface side effects of topical glaucoma medications. However, not all patients achieve sustained IOP control. Around 15% of those undergoing SLT do not respond adequately and may still require multiple drops despite laser treatment.7,8
MIGS: A CONJUNCTIVA-SPARING STRATEGY THAT PROTECTS THE OCULAR SURFACE
MIGS refers to a group of procedures designed to improve aqueous outflow with minimal trauma. Their defining features include:
• Low tissue disruption,
• High safety profile compared with traditional trabeculectomy or tube shunts,
• More predictable recovery, and
• The ability to significantly reduce medication burden.
The evidence consistently shows that trabecular bypass procedures reduce dependence on topical therapy when combined with cataract surgery or performed as standalone procedures.9-11 In practice, many of my patients reduce their medication load by one to two drops long term.
For the patient, this benefit is immediate:
• Less stinging, less redness, and less dryness,
• Better comfort and visual stability, and
• Improved compliance.
For the ocular surface, this reduction is profound. A single preservative-containing drop contributes to measurable epithelial toxicity; three or four drops amplify that effect exponentially.
When we talk about MIGS, there are two categories to consider.
Trabecular micro-bypass MIGS (such as iStent infinite). The iStent infinite and similar devices bypass the trabecular meshwork, facilitating improved physiological outflow via the canal of Schlemm and the collector channels. Typically combined with cataract surgery, they have high safety and excellent long-term tolerability.
Subconjunctival MIGS (such as Preserflo MicroShunt). The Preserflo MicroShunt creates a controlled subconjunctival filtration pathway with a more predictable bleb profile and less surgical trauma than traditional trabeculectomy. These offer greater pressure reduction than transtrabecular stents, while avoiding some of the risks of traditional trabeculectomy and glaucoma drainage devices.
PROTECTING THE CORNEA: WHY EARLIER MIGS SUPPORTS LONG-TERM OCULAR HEALTH
As already mentioned, the cornea is profoundly influenced by chronic topical therapy and surface inflammation. By changing the traditional paradigm of using drops as a first-line therapy and only moving to laser or surgery as a last resort, we reduce the cumulative toxicity to the ocular surface. In my practice, I now consider MIGS surgery much earlier in my treatment algorithm, and particularly for patients with pre-existing dry eye disease, or those who show early signs of ocular surface toxicity, or are intolerant of multiple topical agents.
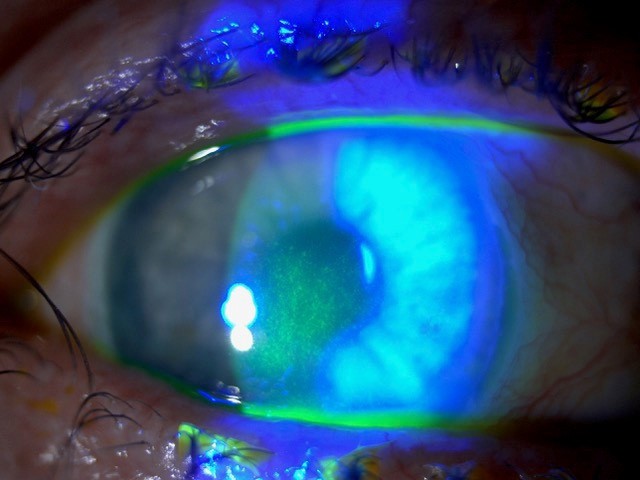
Figure 1. Epitheliopathy caused by chronic drop usage
HOW MIGS HAS CHANGED MY PRACTICE
These real world examples show typical scenarios where drops have failed and MIGS has provided meaningful benefits.
Case 1 — The Polypharmacy Patient
A 74-year-old woman was referred to me for a second opinion with progressive field loss and maximal medical glaucoma treatment, being Xalacom and Simbrinza. However, on further questioning, her main concern was her incredibly sore, red eyes and fluctuating vision. When I asked her what her ocular treatment actually consisted of, it was much more complicated: Celluvisc 4x/day, FML 1x/day, Hylo Forte 6x/day, Ikervis 1x/day, Vita-POS 1x at night, warm compresses 2x/day, Xalacom 1x/day, Simbrinza right 2x/day. To have all this burden of treatment and still be miserable is no way to live. Examination revealed extensive punctate epitheliopathy and signs of chronic conjunctival inflammation, pressures of 20 and 17 mmHg right and left respectively, and moderately advanced glaucoma in the right, more than the left, eye.
After discussion with the patient, my recommendation was to go on a ‘drug holiday’ whereby we ceased all of her topical medications and managed the pressures with low dose oral acetazolamide (Diamox). She felt immediate improvement of her symptoms and told me that the side effects of the Diamox were quite tolerable compared to the ocular surface symptoms caused by the drops. Three weeks later, we proceeded with Preserflo insertion in the right eye. She achieved a pressure of 14 mmHg on no pressure-lowering medications and maintained her ocular surface with warm compresses and 4x/day Hylo Forte only. Subjectively, she felt much more comfortable.
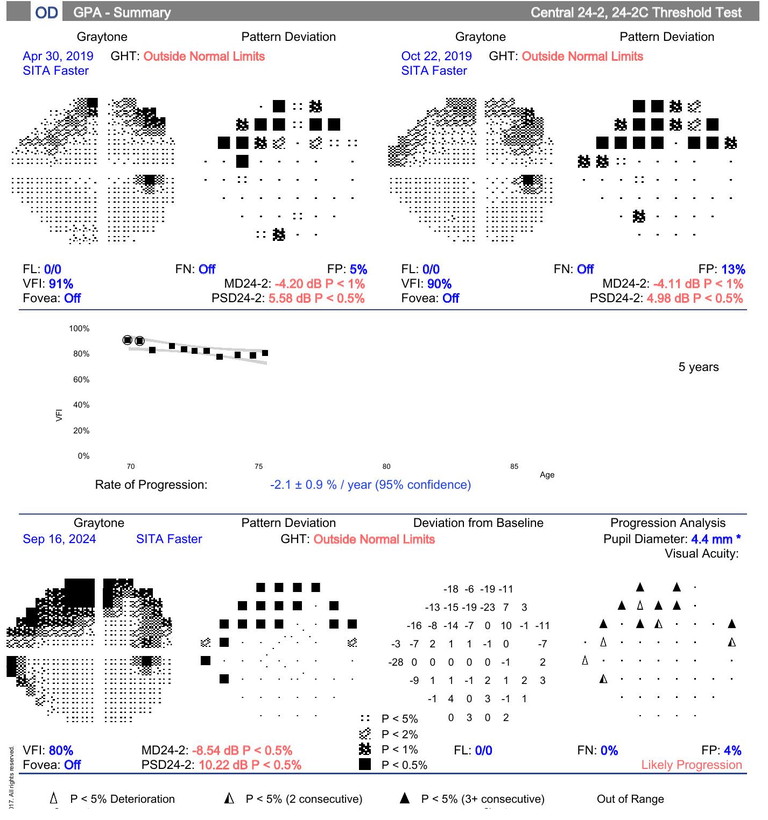
Figure 2. The same patient’s visual field progression analysis, showing progressive field loss and then stabilisation following surgery.
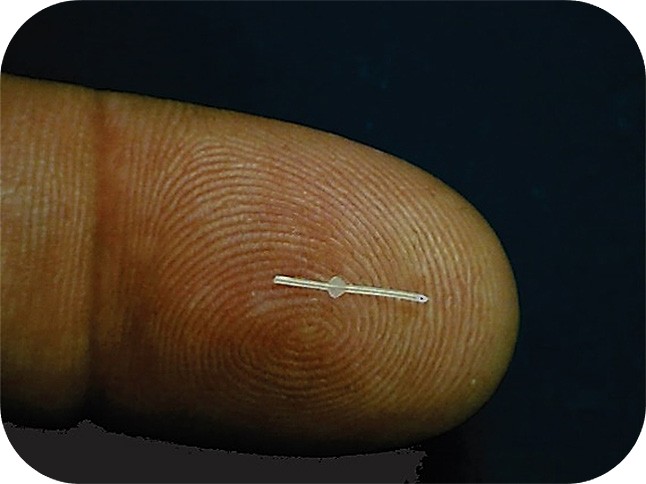
Figure 3. The Preserflo device.

Figure 4. The iStent infinite.
Case 2: Progressive Glaucoma with Surface Intolerance A 69-year-old gentleman was referred to me for diagnosis and management of glaucoma. On examination, he had early primary open-angle glaucoma with a mild inferior arcuate scotoma in the right eye, a normal field in the left eye, and pressures in the mid to low 20s. He also had a history of significant asthma requiring inhaled and occasional oral steroids, contraindicating the use of beta-blockers.
Over about a year, we tried various agents, including preserved and non-preserved prostaglandins, carbonic anhydrase inhibitors, alpha-agonists and SLT laser. All topical agents caused significant redness and irritation, and despite SLT resulting in a drop of pressures to the high teens, there was evidence of further progression of his right field and a suggestion of early field changes in the left. Simultaneously, he was developing some cataract.
We decided to proceed with combined cataract surgery and iStent infinite insertion (which allows for the implantation of three stents). Following this, his pressures stabilised at 14–15 mmHg, the right arcuate scotoma has not progressed and the left field remains normal. Most importantly, every time I see him, he tells me how grateful he is not to have to take “those awful drops”.
HOW OPTOMETRISTS DOVETAIL INTO MIGS CARE
Co-management remains an essential pillar of glaucoma care, and the shift toward early MIGS has only deepened the importance of collaboration between optometrists and ophthalmologists. Optometrists are often the first to detect subtle changes in comfort, compliance or progression, and for many patients, these early observations determine whether they continue years of escalating topical therapy or move toward a strategy that better protects their ocular surface over the long term.
A challenge in primary eye care is that the treatment tools available to optometrists are largely limited to topical medications. SLT and MIGS – two intervention pathways that substantially reduce medication burden – remain outside optometric scope in Australia. As a result, there can be a natural tendency to continue modifying, adding, or persisting with topical agents, even when side effects, intolerance, or progressive disease suggest that drops alone may no longer be the best option. Similarly, many optometrists understandably hesitate to withdraw pressure-lowering therapy, even when ocular surface toxicity is severe, for fear of compromising glaucoma control. Medication withdrawal can be extremely useful in determining the contribution of glaucoma drops to ocular surface symptoms.
We now understand that chronic OSD, conjunctival inflammation, and medication-related discomfort are not just quality-of-life problems – they affect visual fields, compliance, biometry, future surgical outcomes, and the longevity of the ocular surface itself. Early referral avoids the prolonged period of
‘toughing it out’ with drops, and gives patients access to interventions that can stabilise both their pressures and their ocular surface for years ahead.
WHEN TO STOP ESCALATING DROPS AND REFER
Optometrists should consider earlier referral when any of the following are present:
1. Chronic moderate or severe ocular surface disease while on glaucoma drops,
2. Dry eye symptoms not responding as expected to therapy,
3. Progressive glaucoma despite apparently ‘adequate’ pressures,
4. Suboptimal or unstable IOP control,
5. Patients considering cataract surgery where combined cataract and stents is appropriate, and
6. Moderate to advanced glaucoma where significant pressure lowering is needed.
These referral triggers greatly reduce the risk of patients becoming ‘medical failures’ long before they are referred for laser or surgery. Early intervention with SLT or MIGS not only improves pressure control but often leads to a healthier tear film, reduced inflammation, and greater day-to-day comfort – all of which make co-managed care more effective.
COLLABORATIVE CARE BEYOND SURGERY
Ongoing co-management after SLT or MIGS is equally important. Optometrists remain central to monitoring IOP trends, ensuring medication tapering is appropriate, assessing ocular surface recovery, and providing long-term field and OCT surveillance.
The combination of community-based continuity and timely interventional care creates a pathway that is safer, more sustainable and far more comfortable for patients who will be living with glaucoma for the rest of their lives.
CONCLUSION
Glaucoma care is no longer just about protecting the optic nerve; it is about protecting the whole eye over decades of treatment. Chronic topical therapy carries real and cumulative consequences for the ocular surface, conjunctiva, and corneal endothelium. MIGS has given us an opportunity to intervene earlier – not to ‘do more surgery’, but to minimise cumulative harm, preserve tissue, and create healthier long-term outcomes.
By reframing early intervention as a form of ocular surface and corneal preservation, we can offer our patients a safer, more comfortable and more sustainable path through a lifetime of glaucoma management.
This article was sponsored by Glaukos.
To earn your CPD hours from this activity, visit mieducation. com/protecting-the-corneain-glaucoma-why-i-interveneearlier-with-migs.

References available at mieducation.com.

Dr Nicholas Toalster FRANZCO MBBS (Hons) BAppSci Optometry (Hons) is a cataract, cornea, anterior segment, and glaucoma surgeon based in Brisbane. He is a Senior Lecturer at the University of Queensland and operates at the Royal Brisbane and Women’s Hospital and Visionare Eye Specialists, with a particular interest in minimally invasive glaucoma surgery and complex anterior segment reconstruction.