mitechnology
Light-Based Therapy for Dry AMD A Promising Development
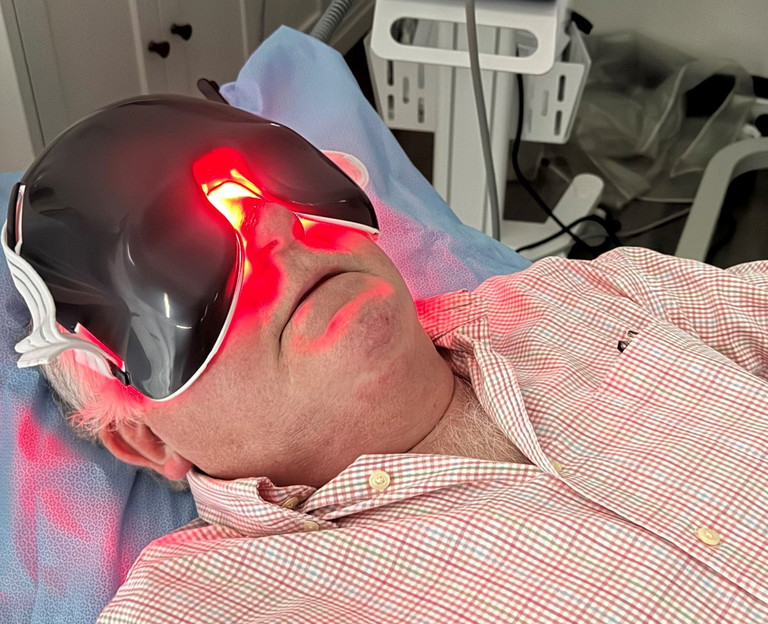
Figure 1. Patient being treated for dry AMD using photobiomodulation therapy.
Over the past decade, researchers have explored new therapeutic strategies to address the underlying cellular damage associated with dry age-related macular degeneration (dry AMD). One emerging treatment is photobiomodulation therapy (PBMT), also known as low-level light therapy (LLLT). This non-invasive treatment uses specific wavelengths of light to stimulate cellular processes within the retina, potentially improving retinal metabolism and slowing disease progression.
PBMT has attracted growing interest in ophthalmology because it targets the metabolic and inflammatory pathways that contribute to retinal degeneration. In this article, Dr Nisha Sachdev, one of the first Australian ophthalmologists to use PBM to treat dry eye disease and meibomian cysts, explores its use for the treatment of dry AMD, including its mechanisms of action, the clinical evidence, treatment protocols, and future potential.
WRITER Dr Nisha Sachdev
One of the earliest clinical signs of dry AMD is the appearance of drusen, small yellow deposits of lipids and proteins that accumulate between the retina and the underlying retinal pigment epithelium (RPE).
Several pathological processes occur with AMD formation:
• Degeneration of the retinal pigment epithelium (RPE),
• Damage to photoreceptor cells,
• Reduced oxygen and nutrient delivery to retinal tissues,
• Chronic inflammation,
• Increased oxidative stress, and
• Impaired mitochondrial function.
In more advanced stages, dry AMD may lead to geographic atrophy – the irreversible chronic loss of the RPE, photoreceptors, and choriocapillaris.
CURRENT TREATMENT LIMITATIONS
Unlike neovascular AMD, which is treated with anti-VEGF injections, treatment options for dry AMD remain exceptionally limited.
The most widely recommended intervention is nutritional supplementation, based on findings from large clinical studies (such as AREDS) showing that certain formulations of antioxidants, vitamins, and minerals may reduce the risk of progression from intermediate to advanced AMD.1,2 For further information read the article on page 73.
However, these supplements do not reverse retinal damage; their primary benefit is in slowing disease progression. Similarly, newly-approved intravitreal injections for geographic atrophic AMD have been shown to slow progression.
Because of these limitations, researchers have increasingly focused on therapies that address the cellular mechanisms underlying retinal degeneration. Photobiomodulation therapy is one such approach that aims to improve retinal cell metabolism, resulting in a reduction in drusen.
WHAT IS PHOTOBIOMODULATION THERAPY?
The concept of photobiomodulation is not entirely new. Light-based therapies have been studied for decades in fields such as dermatology, wound healing, neurology, and musculoskeletal medicine.3-6
In eye health, it has been utilised for dry eye disease, as previously discussed.7 More recently, researchers have investigated its potential benefits for retinal diseases.
PBMT uses low-intensity light at specific wavelengths to stimulate biological processes in cells and tissues. Unlike high-energy lasers used in surgical procedures, PBMT delivers light at levels that do not cause thermal damage or tissue destruction.
The therapy typically uses wavelengths within the visible red and near-infrared spectrum, generally ranging from approximately 590 to 850 nanometers. These wavelengths are able to penetrate biological tissues and interact with cellular components that influence metabolism and signalling pathways.8,9
For use in dry AMD, PBM devices deliver controlled light exposure to the retina with delivery via a mask.10 Treatments are usually administered in the clinical setting and the therapy is non-invasive, painless, atraumatic, and relatively quick (Figure 1).
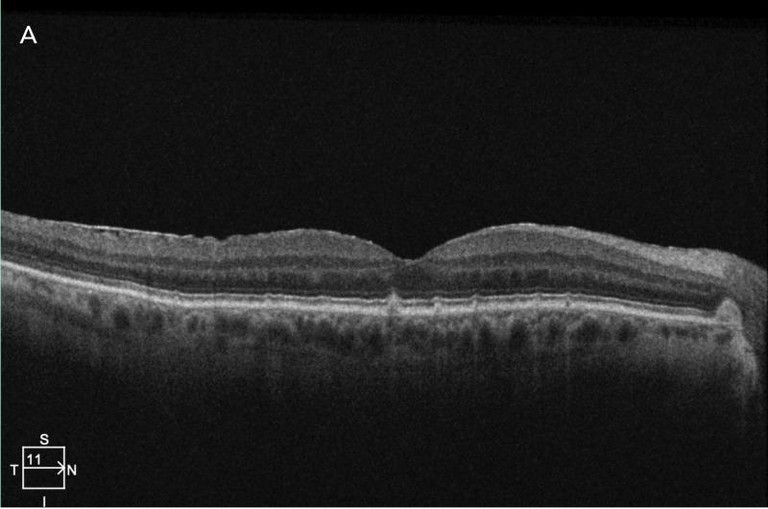
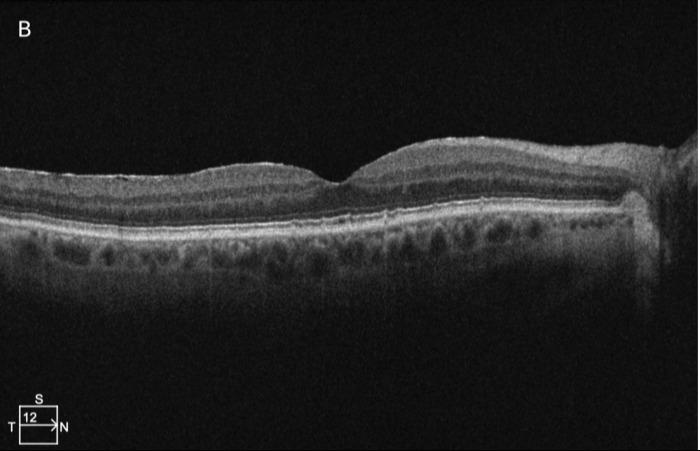
Figure 2. Macular optical coherence tomography of left eye in a 65 year old patient: A. before treatment and B. two months after one cycle of LLLT (using yellow and red light therapy).
“PBMT has the potential to improve retinal health and slow the progression of dry AMD”
BIOLOGICAL MECHANISMS OF PMB FOR DRY AMD
Photobiomodulation therapy, in the setting of AMD, works by influencing several cellular processes that are known to contribute to retinal degeneration.8,11,12 The primary target is the mitochondria, which are responsible for producing energy within cells.
Enhancement of Mitochondrial Function
One of the most widely accepted mechanisms of PBMT involves stimulation of cytochrome c oxidase, an enzyme in the mitochondrial respiratory chain. When this enzyme absorbs light in the red or near-infrared spectrum, it enhances the efficiency of mitochondrial energy production.
This leads to increased synthesis of adenosine triphosphate (ATP), the molecule that fuels many cellular functions. This allows retinal cells to maintain normal metabolic activity and resist degenerative changes.
Reduction of Oxidative Stress
Oxidative stress is a key factor in the development of dry AMD. It occurs when the production of harmful reactive oxygen species exceeds the body’s ability to neutralise them.
Photobiomodulation therapy has been shown to:
• Reduce oxidative damage within cells,
• Improve antioxidant defence mechanisms, and
• Stabilise mitochondrial activity.
By decreasing oxidative stress, PBM therapy may help protect retinal pigment epithelial cells and photoreceptors from damage.
Anti-Inflammatory Effects
Chronic inflammation plays a significant role in the progression of AMD. Inflammatory mediators and immune responses can contribute to retinal cell injury and degeneration. Studies suggest that PBMT may regulate inflammatory signalling pathways, resulting in reduced production of inflammatory molecules and improved cellular homeostasis within the retina.5
Improved Blood Flow and Tissue Oxygenation
Some research indicates that photobiomodulation may enhance microcirculation in retinal tissues.8 Improved blood flow helps deliver oxygen and nutrients to metabolically active cells, supporting retinal health.
Promotion of Cellular Repair and Survival
PBMT can also activate protective cellular signalling pathways that promote cell survival, reduce apoptosis (programmed cell death), and support tissue repair.
Together, these mechanisms may help create a more favourable environment for retinal cells, potentially slowing or stabilising degenerative changes associated with dry AMD.
THE CLINICAL EVIDENCE
Several clinical trials and pilot studies have evaluated the use of PBMT in patients with dry AMD. While research is still evolving, many studies have reported encouraging outcomes.10-16 Some key findings from clinical investigations include:
• Improved visual acuity in certain patients,
• Better contrast sensitivity,
• Reduced drusen volume in some cases, and
• Improved retinal structure observed through imaging techniques.10-16
In many studies, patients received multiple treatment sessions over several weeks.10-16 Improvements in visual function were sometimes observed shortly after treatment, and maintained for several months.
One important observation from clinical trials is that patients with early to intermediate stages of dry AMD tend to respond more favourably than those with end stage or advanced geographic atrophy.10-16
It is important to note that responses can vary between individuals, and not all patients experience the same degree of improvement.
TREATMENT PROCEDURE AND PROTOCOLS
Photobiomodulation therapy is typically performed using specialised ophthalmic devices designed to deliver precise wavelengths of light to the retina.
Although treatment protocols may vary depending on the device and clinical study design, common features include:
• Multiple wavelengths of light (often yellow and red),
• Short treatment sessions, usually lasting a few minutes, with non-pulsed and pulsed components,
• Repeated treatments; often two sessions per week, and
• Treatment cycles lasting several weeks, repeated in a few months.
During the procedure, patients sit comfortably while the device directs controlled light exposure toward the eyes. The treatment is painless and generally well tolerated.
Patients may resume normal activities immediately afterward, as the therapy does not require recovery time.
ADVANTAGES OF PHOTOBIOMODULATION THERAPY
Photobiomodulation offers several potential advantages
• A non-invasive approach (PBM involves only exposure to low-intensity light),
• Minimal side effects,
• A painless treatment,
• Potential neuroprotective benefits: By improving cellular metabolism and reducing oxidative stress, PBMT may help protect retinal cells from degeneration rather than simply managing symptoms, and
• Compatibility with other treatments: Photobiomodulation can potentially be used alongside nutritional supplements and other management strategies.
LIMITATIONS AND CHALLENGES
Despite its promise, photobiomodulation therapy is not yet considered a universal standard of care for dry AMD.
Some important limitations include:
• Variability in treatment protocols across studies,
• Differences in device technology and wavelengths used,
• Limited long-term data regarding sustained benefits, and
• Variation in patient response.
Additionally, PBMT may be less effective in advanced stages of the disease where significant retinal cell loss has already occurred. Further research is needed to determine optimal treatment parameters and identify which patients are most likely to benefit.
THE FUTURE OF PBMT IN OPHTHALMOLOGY
The growing interest in photobiomodulation reflects a broader shift in ophthalmic research toward metabolic and neuroprotective therapies. Future research may focus on:
• Optimising wavelength combinations and energy delivery,
• Determining ideal treatment frequency and duration,
• Identifying biomarkers that predict treatment response, and
• Combining PBMT with emerging therapies targeting retinal regeneration.
Advances in retinal imaging and diagnostic technology may also help clinicians better monitor the effects of PBMT and refine treatment strategies.
As clinical evidence continues to expand, photobiomodulation may become an important component of comprehensive AMD management.
CONCLUSION
Dry age-related macular degeneration remains a major cause of vision loss worldwide, and current treatment options are limited. Photobiomodulation therapy represents an innovative approach that targets the underlying cellular dysfunction associated with retinal degeneration.
By using low-level light to stimulate mitochondrial activity, reduce oxidative stress, and modulate inflammation, PBMT has the potential to improve retinal health and slow the progression of dry AMD. Early clinical studies suggest that this therapy may enhance visual function and stabilise disease in certain patients, particularly those in the early stages.
While additional large-scale clinical trials are needed to fully establish its long-term effectiveness, photobiomodulation therapy offers a promising new direction in the management of dry AMD. As research advances, light-based therapies may play an increasingly important role in preserving vision and improving quality of life for individuals affected by this common retinal condition.
Dr Nisha Sachdev MBChB PhD FRANZCO is a general ophthalmologist and the founder and Director of City West Eye Specialists in Sydney. Dr Sachdev completed her surgical training in ophthalmology in New Zealand and further subspecialty training in Melbourne.
She has been involved in many research projects, has taught registrars, presented at international conferences and published numerous research papers. In addition, she is the youngest ophthalmologist to have received the RANZCO Federal Meritorious Services Award for her RANZCO contributions over the past 20 years.
References available at mivision.com.au.