mipatient
Macular Holes: Pathophysiology, Classification, and Treatment
WRITER Jessica Chi

The development of a macular hole can be distressing for patients, often leading to central visual distortion and reduced vision. Jessica Chi explores the underlying pathophysiology of macular holes, and current classification systems used to stage macular holes; essential for guiding management and prognosis.
Approximately 90% of macular holes are idiopathic. They occur in approximately twice as many women compared to men, with peak incidence in women aged 70–79. An Australian study from Tasmania reported an incidence of full thickness macular holes (FTMH) as four per 100,000.1
Non-idiopathic causes of macular holes are rare under 40 years of age, with causes including trauma, high myopia, post-intraocular surgery, epiretinal membrane, hypertensive, or diabetic retinopathy.
Bilateral cases occur in between 7–12% of patients, with no clear systemic association reported.1,2
PATHOPHYSIOLOGY
With ageing, the vitreous undergoes liquefaction (synchysis) and progressive weakening of the vitreoretinal junction, eventually leading to posterior vitreous detachment (PVD). However, in abnormal PVD, liquefaction occurs but the vitreoretinal adhesion persists.
Persistent adhesion at the macula results in vitreomacular traction (VMT), which deforms the foveal architecture. Continued traction can lead to intraretinal splitting and progressive dehiscence of the retinal layers, which may ultimately result in the formation of a FTMH.
Gass Classification
The original classification of macular holes was described by Gass.
Stage 1. Partial-thickness foveal detachment caused by VMT forming an intrafoveal pseudocyst, which may appear as a central yellow spot on fundus examination. Approximately half resolve spontaneously.
Stage 2. Small (<400 microns) FTMH with persistent VMT.
Stage 3. Large (>400 microns) FTMH with VMT present.
Stage 4. FTMH with complete posterior vitreous detachment (PVD).
A full-thickness macular hole is defined by a defect extending through all layers of the neurosensory retina, from the internal limiting membrane (ILM) to the retinal
pigment epithelium (RPE). Photoreceptor separation leads to significant vision loss.
Without intervention, many stage 2 holes progress to stage 3 holes. Early vitrectomy with gas tamponade reduces progression and improves anatomical and visual outcomes.3
The International Vitreomacular Traction Study Classification
In 2013, the International Vitreomacular Traction Study (IVTS) group created a new classification, based on optical coherence tomography (OCT) findings, to modernise the diagnosis and treatment of vitreomacular interface diseases. The following more precise and standardised definitions are intended to improve clinical decision making and prognosis:4
Vitreomacular adhesion. Vitreous separation around the fovea without distortion of the foveal contour.
Vitreomacular traction. Anatomical distortion of the foveal contour, and intraretinal structural changes without complete separation of the intraretinal layers. These may include pseudocysts, macular schisis, cystoid macular oedema, and subretinal fluid.
Full-thickness macular hole. A defect affecting all retinal layers, from the internal limiting membrane to the retinal pigment epithelium. It is defined as primary when it is caused by VMT, or secondary if from pathology other than VMT.
FTMH is further classified by size of the minimum horizontal diameter: small (< 250 μm), medium (250 to 400 μm), and large (> 400 μm).
Small holes are likely to spontaneously resolve and have the most favourable response to victrectomy and pharmacologic vitreolysis (e.g., ocriplasmin).
MANAGEMENT OF MACULAR HOLES
Early cases of stage 1 macular holes may be managed conservatively with observation and serial OCT monitoring every four to six weeks.
Spontaneous release of VMT occurs in half of these cases, which may restore normal foveal architecture. However persistent traction can progress to a FTMH, warranting treatment in non-resolving cases.
“Continued traction can lead to intraretinal splitting and progressive dehiscence of the retinal layers”
For symptomatic or FTMH, early intervention with pars plana vitrectomy (PPV), posterior hyaloid removal, inner limiting membrane (ILM) peel, and gas tamponade yields a high rate of success. More than 90% of holes are expected to close following a single surgery, with significant improvement in visual acuity and prevention of further disease progression. However, postoperative cataract formation is a common complication.
Alternative Options
Because surgery requires specialised expertise and carries high cost and surgical risk, less invasive treatments have been explored, including pneumatic vitreolysis (PVL) and pharmacological vitreolysis.
PVL involves intravitreal gas injection to induce PVD. Early studies reported resolution of VMT in most cases and closure of approximately half of stage 2 macular holes, however later studies have found a relatively high incidence of macular hole formation, progression, and retinal detachment.5
Pharmacologic vitreolysis involves injecting ocriplasmin – a proteolytic enzyme that breaks down fibronectin and laminin, which are key components of the vitreomacular interface – thereby inducing PVD. However, this has been shown to have varying success. Adverse effects are relatively common, including transient vision reduction, metamorphopsia, and persistent visual disturbances in some patients. There have also been reports of retinal tears and detachments.6
Consequently, many patients who undergo PVL or ocriplasmin injections will still require PPV, making the latter the gold standard treatment.
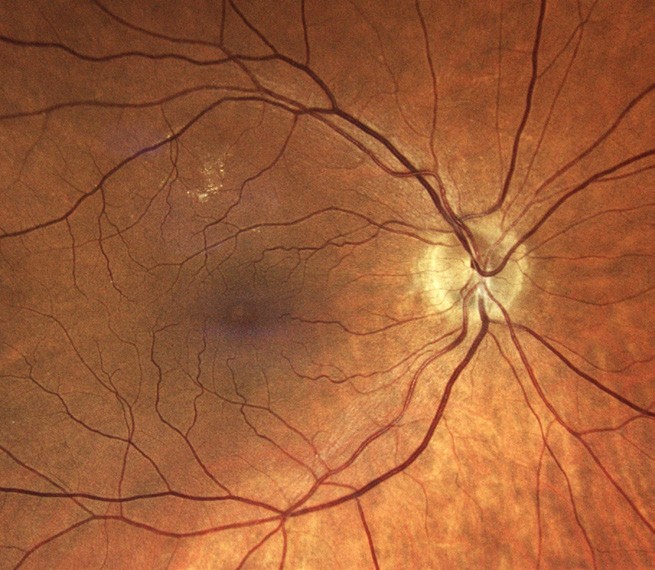
Figure 1. Fundus examination showing macular hole in the right eye with VMT.
“Small holes are likely to spontaneously resolve and have the most favourable response to victrectomy...”
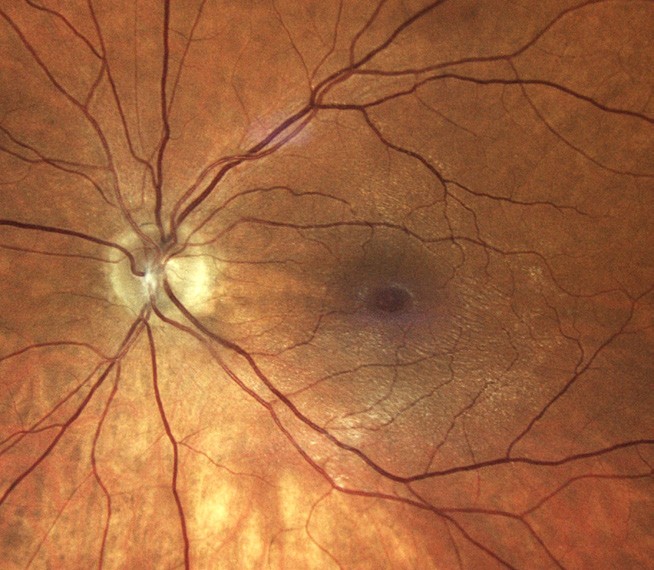
Figure 2. Fundus examination showing macular hole in the left eye with VMT.
CASE STUDY
Alice Leigh,* a 75-year-old female, presented with blurred vision in both eyes over the past few weeks. She reported distorted vision, with lines appearing wavy (metamorphopsia) and did not feel confident driving. She denied any history of ocular trauma or surgery.
Her medical history was significant only for well-controlled hypertension.
Vision unaided was R 6/38, L 6/24=.
Refraction was R -0.75/-0.50x10 (6/24=), L -1.00/-1.50x153 (6/7.5), near add +2.50DS. No improvement was achieved with pinhole.
Anterior eye examination revealed grade 1 nuclear sclerosis bilaterally, but was otherwise unremarkable.
Fundus examination showed round, well-demarcated foveal defects in both eyes, suspicious for bilateral macula holes (Figures 1 and 2).
OCT demonstrated bilateral VMT. The right eye exhibited an oblique stage 2 FTMH
(Figure 3) while the left demonstrated a stage 1 macular hole (Figure 4).
Ms Leigh was referred to a vitreoretinal surgeon. PPV and ILM peel with gas tamponade were planned for the right eye. Given the lesser anatomical and functional impact in the left eye, the plan for the left eye was observation.
Two months following PPV surgery, Ms Leigh returned. She reported her vision had gradually improved. She was no longer aware of any distortions in her vision and she had resumed driving.
Vision unaided was R 6/15, L 6/15.
Refraction was -0.75/-0.50x40 (6/9), L -1.00/-1.50x153 (6/6-).
OCT revealed closure of her right FTMH, with residual foveal subretinal fluid (Figure 5). Fortunately, her left eye demonstrated spontaneous improvement without treatment (Figure 6).
However, the cataract in the right eye had progressed.
*Patient name changed for anonymity.
Jessica Chi is the Director of Eyetech Optometrists, an independent speciality contact lens practice in Melbourne. She is the current Victorian, and a past National President of the Cornea and Contact Lens Society. She is a clinical supervisor at the University of Melbourne, a member of Optometry Victoria Optometric Sector Advisory Group, and a Fellow of the Australian College of Optometry, the British Contact Lens Association, and the International Academy of Orthokeratology and Myopia Control.
References available at mivision.com.au.
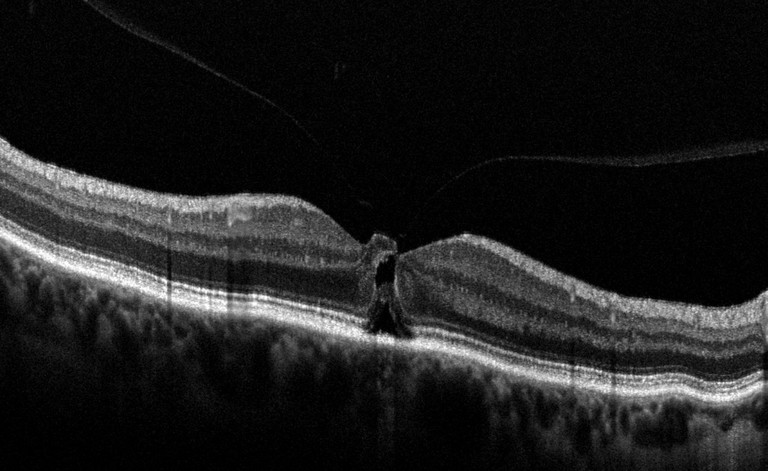
Figure 3. OCT showing full thickness macular hole in the right eye with VMT.
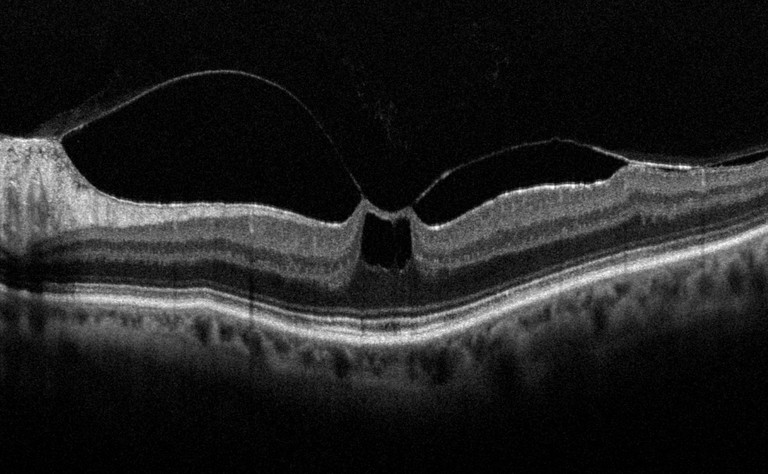
Figure 4. OCT of stage 1 macular hole in the left eye with VMT.
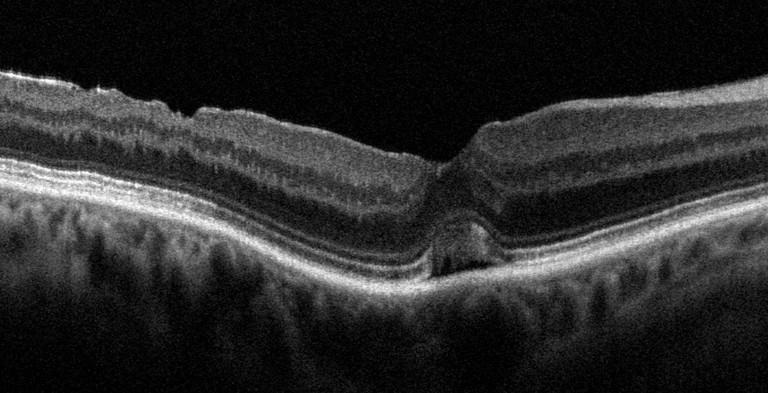
Figure 5. Right macula hole post vitrectomy.
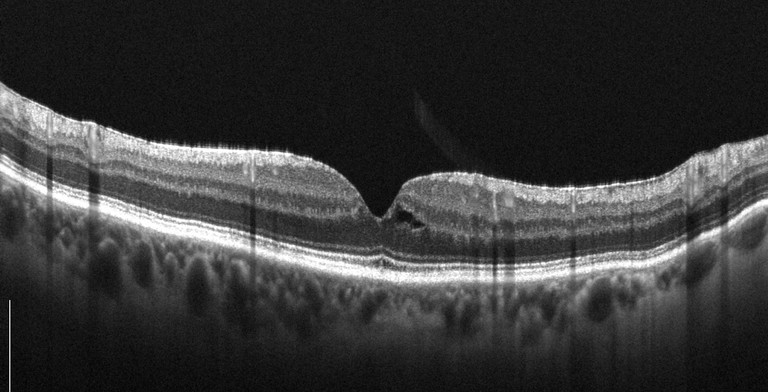
Figure 6. Left eye following spontaneous macular hole recovery.